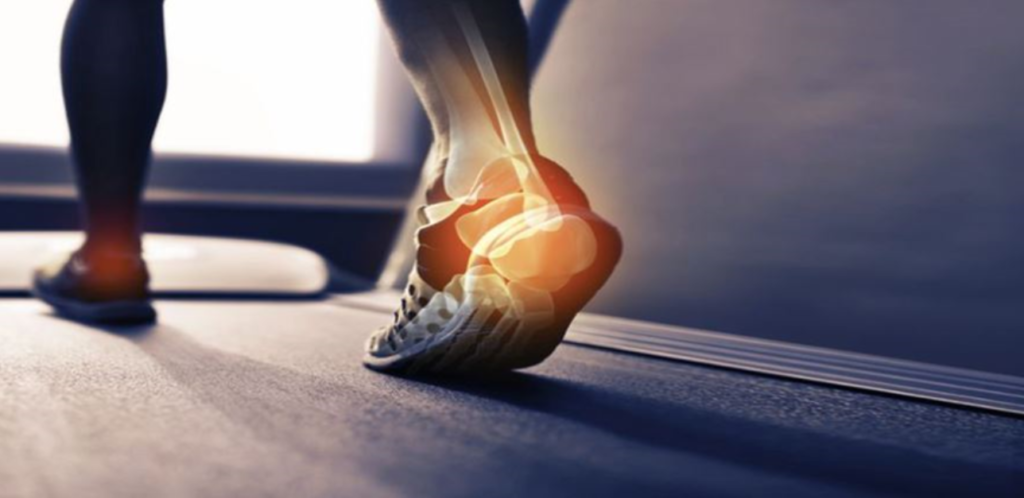
How To Tackle Tarsal Tunnel Syndrome
FOOT PAIN BY NERVE COMPRESSION:
HOW TO TACKLE TARSAL TUNNEL SYNDROME: THE EFFECTIVENESS OF SPORTS PHYSIOTHERAPY TREATMENT & PREVENTION
A SPORTS PHYSIOTHERAPY BASED APPROACH ON LOWER LIMB INJURY & REHABILITATION.
Sports injuries occur when you practice a sport or perform some type of physical exercise under high intensity, extended durations of competition or extreme speeds of movement, such acute injuries or overuse injuries can stem into more complex lower limb conditions. The most common body parts which sustain acute injuries are the pelvis, groin, and leg
Athletes are usually more likely to experience these types of injuries, most commonly are Abductors strains, Plantar Fasciitis, Shin Splints, Anterior Ankle Impingement, Hamstrings, Rectus Abdominal Muscle strain, Hip dislocation amongst others. “Muscles strains injuries are the principal ones amid sports practitioners, representing up to 31% of patients who attend seeking help, and the Adductor muscle injuries represented the second most commonly injury sustained by European football players reaching up to 23% so letting the top spot to Hamstrings injuries which reach up to 37% of prevalence, in other study the results found were that adductor strain/pain accounted 9% to 18% of whole lower limb injuries in pro footballers” John Kiel; Kimberly Kaiser(2020).
In which sports are more likely to go through those kinds of injuries?
Cross fit, Rugby, Soccer, Martial Arts, Running, Basketball and Hockey. Although it is common for lower limb injuries to be sustained in these sports, injury can occur whether by practicing such activities or by doing regular day-to-day tasks during normal lifestyle, it’s completely usual to get injured without having practiced sporting activities too.
Gürhan Dönmez, Savaş Kudaş ET la (2016) stated out on their article about Posterior Ankle Impingement in professional footballers that “Conservative management i.e Physical therapy modalities were greatly efficacious over 2/3 of this (PAI) syndrome among elite footballers, which means 69.2% (18 football players of 26) of reduced complaints treated by non-surgical process whilst the rest 8 individuals (five chronic cases and three acute cases) did not recover completely and surgical management was performed, in as much as posterior ankle arthroscopy is a gold standard procedure when a conservative management does not meet the expectations, every athlete put back to their prior level of proficiency” In this Case Onward referrals to orthopaedic surgeons or musculoskeletal joint specialist are essential in reducing the athletes return to sport. Lower limb pain within sports can be unbearable and debilitating, you always wonder how the extent of damage caused by such blow / tackle it makes you hesitate to decide what to do next?
MY sports Injury | Manchester city
MY SPORTS INJURY | Sports Physiotherapy clinic is an established clinic Located in Manchester City Centre, our Sports Injury Clinic offers high end Manual physical therapy, soft tissue massage, sports injury rehabilitation and myofascial active release therapy.
This blog manu encompasses all the follow-up steps and insights you need as with regards to nerve compression injuries in this particular case the tarsal tunnel syndrome. When the patients show up at MY Sports Injury | Manchester, have team of qualified sports injury professionals and experts in musculoskeletal disorders, efficient and capable sports physiotherapist & sports Therapist practitioners at your assistance to help get the pain away and impairments out to a manageable state in order to live a pain free unrestricted lifestyle and move around with ease.
What’s the structure of the tarsal tunnel?
–This looks to be very interesting, let me explain to you briefly.
The tarsal tunnel is a narrow space located within the ankle next to the ankle bones. The tunnel is overlaid by a thick ligament known as (flexor retinaculum) that protects and holds back the structures (nerves, arteries, tendons, and veins) inside the tunnel. One of those elements is the posterior tibial nerve, a primary focus to tarsal tunnel syndrome.
To put it another way, what’s a tarsal tunnel syndrome about? – What does it appear like? Tarsal tunnel syndrome is the compression or the pinching of the posterior tibial nerve that produces symptoms anywhere to all the way down the nerve. The tibial nerve rear runs inside the ankle towards the foot. Tarsal tunnel syndrome is similar to carpal tunnel syndrome presented on the wrist. Both of these disorders arise from compression of a nerve in a limited space. Even though tunnel syndrome tarsal is not as well-known as the carpal tunnel syndrome, it is still a cause of foot and ankle pain in adults or elite athletes.
“When the Carpal Tunnel Syndrome is tackled and diagnosed ere it becomes an advanced stage, a conservative management as an approach procedure would be prescribed and recommended because its effectiveness, at first moment, the patient has to be aware to stop wrist movements that caused symptoms pain, for example, to place the keyboard height on a sustainable and reasonable elevation and dodge the flexion, abduction, adduction and extension of the damaged hand at typing. The recommendation is to avoid unnecessary motion as much as possible, the use a wrist night-splint can be suggested as well, these advices and recommendations got to be attached to a hand therapist specialist counselling, besides turn up to manual physical therapy sessions, in the other hand in cases were the pain is not being eased a short string doses of non-steroidal anti-inflammatory drugs will be referred, last shot to get rid carpal tunnel syndrome off is surgical management which it’s effective, too” Cited from Matthew Varacallo, Justin O. Sevy (2020).
What are the signs and symptoms of TTS? – How to recognise them. Patients suffering from the syndrome tarsal tunnel sustain one or more of the following symptoms:
• Burning,
• Tingling, a sensation alike an electric shock.
• Numbness.
• Pain, even stabbing pain.
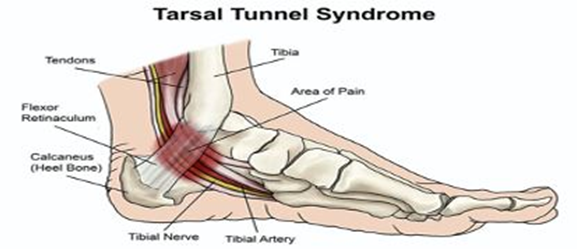
Symptoms are generally perceived inside the ankle and / or on the sole of the foot. In some people the symptoms can be isolated and appear only in one place. In others, they can extend to the heel, arch, toes, and even the calf. Sometimes the symptoms of the syndrome come on suddenly. They are often caused or aggravated by abusive use of the foot, such as standing, walking or exercising for a long time, or starting a new exercise program.
It is essential to start treatment early on at your local Manchester sports physiotherapy clinic if it occurs any of the symptoms of tarsal tunnel syndrome. If not treated, the condition progresses and can result in permanent nerve damage. Additionally, since the symptoms of (TTS) can be confounded with other conditions, an adequate evaluation is key to make a correct diagnosis.
According to D L Jackson and B L Haglund (1992) “(TTS in runners) diagnosis method needs to be extremely accurate in order to stand out and evidence the difference from other similar conditions symptoms presented such as Achilles Tendinitis and Plantar Fasciitis, its treatment generally is a conservative management which normally is acutely successful and effective”
What to know about the causes of TTS? – There’s a large variety of causes, such as:
TTS is produced by anything that causes tightness of the posterior tibial nerve, for examples:
· An injury, such as a sprain, a tackle, a blow can cause inflammation and swelling in or near the tunnel, resulting in compression of the nerve.
·An overweight person is prone to experience pressure on the posterior tibial nerve.
·Systemic diseases such as diabetes or arthritis can cause inflammation and thus compress the nerve.
MY sports Injury | Manchester city provides a high quality level of expertise and experience within professional sports, allowing the sports player / patient to get an accurate clinical diagnosis. MY Sports Injury & physiotherapy clinic allows you to assist your tarsal tunnel syndrome to finally have a full sports recovery, enabling the patient to recover efficiently and safely in accordance to self-management protocols post tarsal tunnel syndrome condition.
Can TARSAL TUNNEL SYNDROME go away on its own?
Compression of the tibial nerve can occur when the ankle is fractured, due to rheumatoid arthritis, foot deformities or demanding physical exercise such as football, basketball, running, rugby and others. Same as Plantar fasciitis which is the inflammation of the fibrous tissue (plantar fascia), which covers the sole of the foot, from the heel to the toes. Prolonged standing, running, and excessive weight can damage the fascia.
According to the (FHSQ) Foot Health Status Questionnaire a study was made about what is Plantar Fasciitis’ effect on the lifestyle’s quality of female and male patients, presented by Patricia Palomo-López, Ricardo Becerro-de-Bengoa-Vallejo ET la (2018) “One hundred patients were recruited 49 males and 51 females with (PF) inflammation, the results of the female patients showed greater vulnerability and worse quality of life than the results shown by the male patients related to foot function, foot pain, general foot health, physical activity, vigor and social capacity”.
Rheumatic syndromes of the soft tissues of the lower limbs (tarsal tunnel syndrome and plantar fasciitis) are very common in people who are rather healthy. Sometimes they go away on their own over time. In most cases, the sports physiotherapy specialist practitioner can treat these types of disorders. Some athletes / patients will need to see a rheumatologist (a specialist in arthritis, rheumatic conditions, and related musculoskeletal conditions) for treatment.
So What are its treatment choices? – Treatment options for TTS When it’s assessed, diagnosed and tackled at an early stage the treatment options for excellence indicated to this syndrome are rest, ice, compression, and elevation known by its acronym (RICE).
Medicine without a preion such as (NSAID) non-steroidal anti-inflammatory drugs, ibuprofen and acetaminophen can be administered to decrease the pain and the symptoms will be more handle-able.
In some chronic pain severe cases, there are other ways to tackle the tarsal tunnel syndrome such as, corrective devices, physical therapy, sports physiotherapy in Manchester or sports massage clinics and in the worst cases must be an onward referral to an orthopaedic surgeon fellow which will continue to perform a non-conservative management.
“Tarsal tunnel syndrome incidence is undefined. This is an often undiagnosed and rare affection with a higher rate of prevalence amid female patients and could be sustained at any age. The non-conservative process success ranking varies from 46% to 96% of the cases and it’s indicated when the non-operatively management such as physical therapy, sports massage. Corrective devices shown to be less effective, it was proven that the outcomes were better in younger individuals who underwent minor symptoms and had a clear etiology and in those when the condition was treated at an early phase, and no prior ankle pathologies, so an early and accurately diagnosis is key” quoted from John Kiel; Kimberly Kaiser (2020).
How long does TARSAL TUNNEL SYNDROME take to heal? – Shall be I back on the sports field /work soon? It’s a frequent question that our patients have in their mind.
Non-severe cases can be treated with (RICE) and without preion medicine, (OTC) also known as over-the-counter medicine. These minor cases of Tarsal Tunnel Syndrome can get better within 48 hours meaningfully with the previous treatment options touched on. Meanwhile, if you do not seek assistance when there are symptoms at a premature phase and let the time pass by then the nerve damage will be permanent.
“108 ankles distributed 72 patients were assessed; the rate age was forty-nine years. The symptoms of the previous surgical process had a 31 months recurrence. Average time for return to an utterly and painless level of capacity was 9 months, every individual had a twelve months follow up” Pointed out by G James Sammarco, Laurette Changon (2003) Outcome, Follow-up and Outlook of Tarsal Tunnel Syndrome approached by surgical management.
Tarsal Neuropathy and how is it caused? – Is there any difference between TTS and Anterior Tarsal Tunnel Syndrome?
Anterior Tarsal Tunnel Syndrome is an uncommon and seldom entrapment neuropathy dysfunction of deep peroneal nerve situated beneath the extensor retinaculum of the ankle. Also called as (DPN) deep peroneal nerve entrapment brought about by the tight fascia band located in the anterior ankle. “Yassin and others notified that twelve out of thirteen patients (92.31%) presented a greatly amelioration of DPN condition after carrying out the surgery” Michael D. Gibboney and Mark A. Deyer (2020).
How do you fix TARSAL TUNNEL WITH SELF MANAGEMENT TIPS?
As we mentioned it before the most common options to fix TTS are: RICE, OTC, Full immobilization as self-management tips but when pain starts to worsen you should be able to look for other possible treatments such as Injection therapy, Physical Therapy, Corrective shoes and Orthopaedic devices, Ultrasound Therapy, Reducing Foot Pressure, Acupuncture sessions at physical therapy centre, Taping or Bracing, Manual Therapy, sports massage / deep tissue massage. Moreover, you can include some exercises to your self-management routine to enhance your TTS and relieve pain such as ankle pumps, eversion or inversion circles, balance exercises, pencil toe lifts, plantar fascia strength, and many more which will be explained in detail by sports physiotherapy specialist / physician practitioner at the moment you attend to your medical consultation at sports physiotherapy clinic in Manchester City Centre.
“Achilles tendinopathy (AT) has a tremendous prognosis with an early initial driving, its management can be divided into two options: conservative and non-conservative. One of these chances must take into account depending of the pain scale whether acute or chronic, but when it’s whole torn there is not another way except for surgery management, conservative therapy is indicated in first line of management and add in the next recommendations: shortening of physical activity levels, preion of (NSAID), eccentric stretching exercises as a complementary tool of physiotherapy can reach up to 40% of pain reduction” Usker Naqvi and Miguel A. Medina Pabón (2020).
How to identify nerve damage within the foot? – What are the tests to run in order to diagnose correctly TTS?
A meticulous assessment will be performed by your healthcare team providers such as manual therapy givers, sport massage practitioners, physical therapy clinicians and acupuncture practitioners at Manchester city physical therapy centre. MY sports Injury which team can assist in a clinical diagnose without any doubt your condition and to assess the nerve damage inner your foot. diagnostic tests will run, those are; nerve conduction velocity (EMG/NCV), magnetic resonance imaging or MRI, X-ray and electromyography which require an onward referral.
REFERENCES
·Calvo-Lobo C, Painceira-Villar R, López-López D, García-Paz V, Becerro-de-Bengoa-Vallejo R, Losa-Iglesias ME, Palomo-López P. Tarsal Tunnel Mechanosensitivity Is Increased in Patients with Asthma: A Case-Control Study. J Clin Med. 2018 Dec 12;7(12)
· Stødle AH, Molund M, Nilsen F, Hellund JC, Hvaal K. Tibial Nerve Palsy After Lateralizing Calcaneal Osteotomy. Foot Ankle Spec. 2019 Oct;12(5):426-431.
· Zuckerman SL, Kerr ZY, Pierpoint L, Kirby P, Than KD, Wilson TJ. An 11-year analysis of peripheral nerve injuries in high school sports. Phys Sportsmed. 2019 May;47(2):167-173.
· Rinkel WD, Castro Cabezas M, van Neck JW, Birnie E, Hovius SER, Coert JH. Validity of the Tinel Sign and Prevalence of Tibial Nerve Entrapment at the Tarsal Tunnel in Both Diabetic and Nondiabetic Subjects: A Cross-Sectional Study. Plast Reconstr Surg. 2018 Nov;142(5):1258-1266.
· Hong CH, Lee YK, Won SH, Lee DW, Moon SI, Kim WJ. Tarsal tunnel syndrome caused by an uncommon ossicle of the talus: A case report. Medicine (Baltimore). 2018 Jun;97(25):e11008.
· Komagamine J. Bilateral Tarsal Tunnel Syndrome. Am J Med. 2018 Jul;131(7):e319.
· Schuh A, Handschu R, Eibl T, Janka M, Hönle W. [Tarsal tunnel syndrome]. MMW Fortschr Med. 2018 Apr;160(6):58-59.
· Mansfield CJ, Bleacher J, Tadak P, Briggs MS. Differential examination, diagnosis and management for tingling in toes: fellow’s case problem. J Man Manip Ther. 2017 Dec;25(5):294-299.
· Tu P. Heel Pain: Diagnosis and Management. Am Fam Physician. 2018 Jan 15;97(2):86-93.
